Unless you’ve been completely offline for the past two years, you’ve heard about Ozempic, Wegovy, and Mounjaro. These GLP-1 and dual GIP/GLP-1 medications have gone mainstream in a way few prescription drugs ever do. Celebrities discuss them openly. Social media is flooded with transformation stories. Conversations about weight loss and obesity have fundamentally shifted.
But behind the brand names and hype, what exactly are GLP-1 peptides? If you’re new to the topic, it helps to first understand what peptides are and how they function in the body. How do they work? And what should you understand before considering them?
This guide explains the science behind GLP-1 receptor agonists, the different medications available, who they’re appropriate for, potential side effects, cost considerations, and what happens long term.
What Are GLP-1 Peptides?
GLP-1 medications are very different from experimental compounds like BPC-157 or TB-500, which are not FDA-approved and have limited human research. GLP-1 stands for glucagon-like peptide-1. It’s a hormone your body naturally produces in the intestines after you eat. Its primary role is regulating blood sugar and appetite.
Naturally occurring GLP-1:
- Stimulates insulin release when blood sugar rises
- Slows gastric emptying (how quickly food leaves the stomach)
- Reduces appetite through effects on brain receptors
- Lowers glucagon secretion (a hormone that raises blood sugar)
In people with type 2 diabetes, GLP-1 signaling is often impaired. That’s why synthetic versions were originally developed to treat diabetes.
GLP-1 receptor agonists are synthetic peptides designed to mimic natural GLP-1 — but with a much longer duration of action. Instead of lasting minutes like the natural hormone, these medications last days.
The Main GLP-1 Medications
Several GLP-1 receptor agonists are FDA-approved and available by prescription.
Semaglutide
- Brand names: Ozempic (diabetes), Wegovy (weight loss)
- Dosing: Once-weekly injection
- Approved: Ozempic (2017), Wegovy (2021)
Tirzepatide
- Brand names: Mounjaro (diabetes), Zepbound (weight loss)
- Dosing: Once-weekly injection
- Approved: Mounjaro (2022), Zepbound (2023)
- Unique feature: Dual agonist (activates both GIP and GLP-1 receptors)
Liraglutide
- Brand names: Victoza (diabetes), Saxenda (weight loss)
- Dosing: Daily injection
- Older generation, now less commonly used due to daily dosing
Dulaglutide
- Brand name: Trulicity
- Primarily used for diabetes
- Once-weekly injection
Semaglutide and tirzepatide are currently the most widely used due to convenience and significant weight loss results in clinical trials.
How Do GLP-1 Medications Work for Weight Loss?
These drugs were developed for diabetes — not weight loss. But consistent weight reduction in clinical trials led to formal obesity treatment approvals.
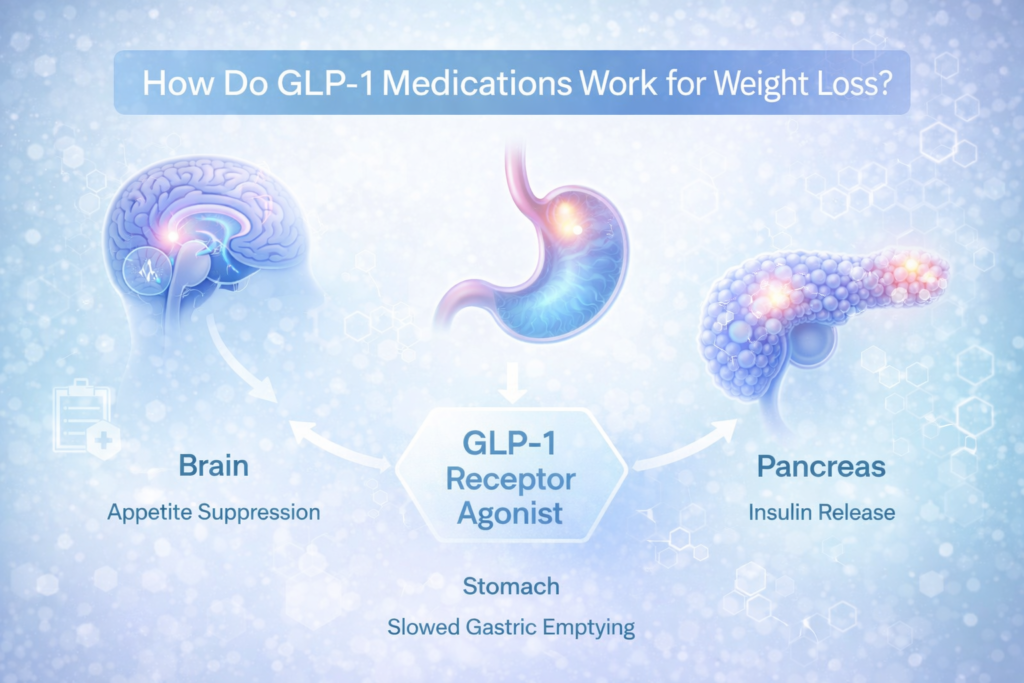
They support weight loss through several mechanisms:
Appetite Suppression
GLP-1 receptor agonists act on brain regions that regulate hunger and satiety. Many users report reduced hunger and feeling satisfied with smaller portions.
Slowed Gastric Emptying
Food remains in the stomach longer, increasing fullness and decreasing overall intake.
Reduced “Food Noise”
A commonly reported effect is reduced intrusive thoughts about food, cravings, and constant mental preoccupation with eating.
Improved Insulin Sensitivity
Better blood sugar control can indirectly improve metabolic health and fat regulation.
The combination makes maintaining a caloric deficit significantly easier than relying on willpower alone.
What the Research Shows
The clinical trial data for semaglutide and tirzepatide is extensive.
Semaglutide (STEP trials)
- Average weight loss: 15–17% of body weight over 68 weeks
- Average loss: ~33–35 pounds
- ~50% of participants lost at least 15% of body weight
- Improvements in cardiovascular risk markers
Tirzepatide (SURMOUNT trials)
- Average weight loss: 20–22% of body weight
- Some participants lost 25%+ at higher doses
- Superior weight loss compared to semaglutide in head-to-head trials
- Significant metabolic improvements
Important context:
- Participants received lifestyle counseling
- Real-world results may vary
- Weight regain is common if medication is discontinued
- Long-term data beyond 5 years is still limited
These are among the most effective medical weight loss interventions ever studied.
Are GLP-1 Peptides Legal?
Unlike many experimental peptides discussed online, GLP-1 receptor agonists such as semaglutide and tirzepatide are FDA-approved prescription medications. If you’re curious how this differs from research peptides sold online, you can read more in our guide to whether peptides are legal in 2026.
Who Are GLP-1 Medications For?
GLP-1 receptor agonists are FDA-approved under specific criteria.
Approved for weight management if:
- BMI ≥30 (obesity), OR
- BMI ≥27 (overweight) with at least one weight-related condition
Also appropriate for:
- Type 2 diabetes
- Cardiovascular risk reduction in certain populations
Not recommended for:
- Personal or family history of medullary thyroid carcinoma
- Multiple endocrine neoplasia type 2
- Pregnancy or planned pregnancy
- History of pancreatitis (use caution)
- Severe gastrointestinal disease
These are prescription medications requiring medical supervision. They are not intended for minor cosmetic weight loss.
Side Effects and Risks
GLP-1 medications are generally well tolerated, but side effects are common — especially during dose escalation.
Most Common (Gastrointestinal)
- Nausea
- Vomiting
- Diarrhea
- Constipation
- Abdominal discomfort
- Bloating
These typically improve over time. Gradual dose increases reduce severity.
Other Reported Effects
- Fatigue
- Headaches
- Dizziness
- Injection site reactions
- Temporary hair thinning (often related to rapid weight loss)
Serious but Rare Risks
Pancreatitis – Severe abdominal pain requires immediate evaluation.
Gallbladder issues – Rapid weight loss increases gallstone risk.
Thyroid tumors (animal data) – Rodent studies showed C-cell tumors. Relevance to humans remains unclear, but medications carry a boxed warning.
Gastroparesis concerns – Severe delayed stomach emptying has been reported in rare cases.
Other considerations include muscle loss during rapid weight reduction and interactions with certain oral medications.
Cost and Access
Cost remains a major barrier.
Typical retail pricing:
- Wegovy: $1,300–1,500/month
- Ozempic: $900–1,000/month
- Mounjaro/Zepbound: $1,000–1,200/month
Insurance coverage:
- More common for diabetes
- Inconsistent for weight loss
- Often requires prior authorization
Manufacturer savings programs can significantly reduce cost for eligible patients with commercial insurance.
Compounded versions exist but are controversial. The FDA has issued warnings about compounded semaglutide and tirzepatide products.
What Happens When You Stop?
This is often overlooked.
Evidence suggests:
- Weight regain is common
- Many regain 50–70% of lost weight within a year
- Appetite and food preoccupation often return
- Metabolic benefits may reverse
Obesity is a chronic biological condition. Removing treatment often allows underlying drivers to re-emerge.
For many individuals, long-term use produces better outcomes than short treatment cycles.
Some people maintain results after stopping by building strong lifestyle foundations during treatment, but this varies significantly.
Lifestyle Changes Still Matter
GLP-1 medications are powerful tools — not standalone solutions.
Key areas to prioritize:
- Nutrient-dense eating
- Adequate protein intake
- Strength training to preserve muscle mass
- Sleep and stress management
- Addressing emotional eating patterns
These medications can make habit change more achievable, but they do not replace it.
The Bottom Line
GLP-1 receptor agonists represent a major advancement in obesity treatment. Clinical evidence is strong. For medically appropriate candidates, they can significantly improve weight, metabolic health, and cardiovascular risk.
However, they involve side effects, high costs, and often long-term commitment.
They are most effective when combined with lifestyle improvements and medical oversight.
If you’re considering GLP-1 medications:
- Discuss eligibility with your physician
- Understand the likelihood of long-term use
- Prepare for potential side effects
- Plan financially
- Use the treatment window to build sustainable habits
Used thoughtfully, GLP-1 peptides can be transformative — but they are not magic, and they are not risk-free.
Frequently Asked Questions
Are GLP-1 peptides safe long term?
Long-term safety data beyond several years is still developing, but current evidence supports their safety under medical supervision.
Do you regain weight after stopping GLP-1 medications?
Many people regain weight if the medication is stopped without ongoing lifestyle support.
Are GLP-1 peptides the same as Ozempic?
Ozempic is a brand name for semaglutide, which is a GLP-1 receptor agonist.

